Work-related determinants of multi-site musculoskeletal pain among employees in the health care sector
Abstract
BACKGROUND:
Work-related musculoskeletal pain is a major occupational problem. Those with pain in multiple sites usually report worse health outcomes than those with pain in one site.
OBJECTIVE:
This study explored prevalence and associated predictors of multi-site pain in health care sector employees.
METHOD:
Survey responses from 1348 health care sector employees across three organisations (37% response rate) collected data on job satisfaction, work life balance, psychosocial and physical hazards, general health and work ability. Musculoskeletal discomfort was measured across 5 body regions with pain in ≥ 2 sites defined as multi-site pain. Generalized linear models were used to identify relationships between work-related factors and multi-site pain.
RESULTS:
Over 52% of the employees reported pain in multiple body sites and 19% reported pain in one site. Poor work life balance (PRR = 2.33, 95% CI = 1.06–5.14). physical (PRR = 7.58, 95% CI = 4.89–11.77) and psychosocial (PRR = 1.59, 95% CI = 1.00–2.57) hazard variables were related to multi-site pain (after controlling for age, gender, health and work ability. Older employees and females were more likely to report multi-site pain.
CONCLUSION:
Effective risk management of work related multi-site pain must include identification and control of psychosocial and physical hazards.
1Introduction
Musculoskeletal disorders (MSDs) are a major occupational health and safety problem in both developing and developed countries [1, 2]. Prevalence rates of MSDs have increased by 45% over the past20 years [3] despite significant attempts at reducing their incidence. MSDs are complex with multiple causal pathways and pain is often reported in more than one site [4]. Worse health outcomes have been reported for those who report pain in multiple sites compared to those with only one pain site [5–7]. This limited progress in reducing MSD prevalence suggests current approaches to MSD risk management need reassessment [8]. This paper aims to contribute additional insights to this important area by investigating the relevant work place predictors of multi-site pain in a population of health care sector employees.
Prevalence rates of multi-site pain have been reported between 54–84% [5, 9–11] depending upon the definition of multi-site pain used. One population-based study reported that pain in one site did not predict disability risk but when pain was part of a more general pain condition (in multiple sites), disability risk was increased [12]. Multi-site pain has been associated with higher levels of workplace disability (absenteeism, sick leave), and more frequent consultations with primary care practitioners [13] compared to those reporting pain in only one area [5, 14, 15]. Others have reported associations between multi-site pain and adverse effects on non-work activities [12, 16].
Working lives will need to be extended to manage the impact of population ageing [17]. Ensuring individuals have the capacity to continue working is critical to enable an extended working life [18]. Higher rates of multi- site pain have been reported in older workers compared to their younger counterparts [15, 19]. In addition, some studies have reported high numbers of workers leaving work prior to official retirement ages due to musculoskeletal problems [20–22]. Those aged between 51–62 employed in physically demanding occupations have reported MSD prevalence rates 15% higher than their more sedentary counterparts [23]. However, the relationship between age and multi-site pain is not clear-cut and some inconsistencies have been reported. Yeung and colleagues [11] reported that age was significantly associated with pain in two to three body regions. Coggon et al. [19] reported that older employees (50–59 years) had a high prevalence of multi-site pain (adjusted prevalence rate ratio (PRR) = 2.6, 95% confidence interval = 1.9–3.7). In contrast, some studies have reported higher prevalence of multi-site pain among younger employees [14, 24].
In order to effectively manage risks associated with multi-site pain accurate identification of all relevant workplace hazards is required [5, 19, 25, 26]. This may entail different approaches to those currently used to manage MSDs; however, greater clarity is needed about the relative importance of association of work-related factors with multi-site pain to assist with the development of appropriate tools to assist with risk management [8]. Most research in multi-site pain has been undertaken in a European context, with some exceptions [11, 27]. The Australian context remains relatively unexplored. Whilst a large body of literature supports the link between work-related factors-physical and psychosocial-with MSDs [28–31] less has been reported about the relationship between these factors and multi-site pain [24, 32]. The current study aims to address this gap through determining the prevalence of multi-site pain in Australian health care sector employees. In addition, the relationship between work-related factors, age, gender and multi-site pain will be explored.
2Methods
2.1Participants and procedure
Two large hospital networks and one ambulance service in Melbourne, Australia participated in the current study. In 2011, a total of 3643 questionnaires were sent to all employees in selected occupational groups (Paramedics, allied health, patient orderlies, food services assistants, cleaners and allied health personnel), with a 37% response rate (N = 1348). General reminders were sent to participants, these could not be personalised as the questionnaires were sent anonymously. Mean age of respondents was 41.5 years (SD = 11.6, Range 19–74). Older workers were defined as 45 years or older [33].
Ethics approvals were obtained through La Trobe University (FHECC11/54) and the health care organisations involved.
2.2Measurement of variables
A previously administered questionnaire was used in this study [34]. Measures of age, gender, discomfort/pain, workplace physical and psychosocial hazards, general health, work ability, job satisfaction and work life balance are included.
2.2.1Discomfort/pain
Frequency of discomfort/pain rating was recorded separately for five body regions with a question “how often have you felt discomfort or pain in the past six months?” The replies were from 0 to 4 (0 = never to 4 = almost always). Scores for each body region were dichotomised at the median [24] (less than median: 0 = mild; more than median: 1 = severe). Cut-off or the median values for neck and shoulder, hands and fingers, arms, middle to lower back, and hips bottom, legs, and feet were 2, 1, 1, 2 and 2, respectively. Dichotomised variables were summed to express a variable representing the number of areas reported with severe pain. In order to examine pain in multiple body sites, the resultant variable was categorized into two. Multi-site pain was defined as those respondents with 2 or more areas of pain [5]. Zero or one was considered as not having multi-site pain.
2.3Work-related variables
2.3.1Psychosocial hazards
Psychosocial hazards were assessed using a modified version (26-items) of the Work Organisation Assessment Questionnaire (WOAQ) [35]; two items on work life balance were removed, which pilot testing had shown were difficult to understand. Samples items include: Please rate how good or bad, over the last 6 months the following has been: “your pace of work”, “your workload”. Responses were measured from 1 to 5, major problem to very good. Results were categorized using tertile values (low, medium, high). Cronbach’s alpha for psychosocial hazard was 0.94.
2.3.2Physical hazards
Physical hazards were measured with a question “how much of the time (last 6 months) do you … .” and 12 items were included (e.g. you do very repetitive work – repeating same actions every few secs or mins, work in twisted or awkward postures? or push or pull things, using some force?) replies were measured from 1 (never or hardly ever) to 5 (= almost all the time). Summing of all 12 items created the composite variable, a categorical variable was created using tertile values (low, medium, high). Cronbach’s alpha was 0.84
2.3.3Hazardous personal states
Participants were asked to rate their general health from 1 (poor) to 5 (excellent). For this analysis three categories were created by combining 1 and 2 ‘poor’, 3 as ‘good’ and 4 and 5 ‘very good’. Work ability was assessed with a single question asking respondents to rate current work ability compared to their own lifetime best (i.e. with the question “Assume that your work ability at its best has a value of 10 points. How many points would you give your current ability to work? (0 means that you cannot currently work at all, 10 means working ability is at its best”). Scores range from 0 (cannot currently work at all) to 10 (ability to work is at its best) and was categorized into excellent (score 10), good (score 9), moderate (score 7 to 8) and poor (scores 0–6) work ability consistent with others reporting of the measure [5].
Single item measures of job satisfaction and work life balance were also included. Questions were “How happy are you with your job here, as a whole. taking everything into account?” and “How satisfied are you with the balance between your home life and work – considering how much time and energy you have?”. Response options ranged from very dissatisfied (1) to highly satisfied (5), a categorical variable was created using tertile values (low, medium, high).
2.4Statistical analysis
Prevalence rates of musculoskeletal pain in single and multiple sites were calculated (see Table 1). Chi-squared testing was used to determine differences in pain reporting between gender and age (younger and older employees). Significance level was set at 0.05. Generalized linear models with binary logistic assumption were used to calculate the prevalence rate ratios (PRR) and their 95% confidence intervals (CIs) for the relationship between individual, physical and psychosocial factors at work for multi-site pain. All possible determinants (work-related, health and work ability) were first examined in bivariate and then multivariate models. Risk factors were fitted to a model to calculate the association of work related variables with multi-site pain in three different models. Model 1 examined bivariate associations of variables with multi-site pain, Model II and III examine multivariate associations. For items with missing values on less than 5% of cases, the missing value was replaced with sample mean scores by organisation [36]. All statistical analysis was performed using statistical software SPSS version 21. PRRs and 95% confidence intervals (CIs) were used as a measure of association.
3Results
3.1Prevalence of multi-site pain
Prevalence of musculoskeletal pain is shown in Table 1 for single and multiple body sites. Of those who reported having some discomfort, 71% reported pain in at least one body area with 52% of this group reporting pain in two or more body regions.
Areas of pain most commonly reported were arms, hand/fingers and middle/low back pain across all respondents (Table 1). Examination of pain distribution by gender affords a different pattern. For women, the most frequently reported area of discomfort was hand and finger pain, whilst for men it was arm pain.
Significantly higher numbers of women (56%) reported pain in multiple body sites compared to men (50%). Older employees (58%) were more likely to report multi-site pain than their younger counterparts (see Table 2). Across all respondents pain was most commonly reported in the upper limbs (hands/fingers and arms). Distribution patterns differed by gender, more women reporting neck and shoulder pain (44%) compared to men (36%), and also more hip and leg pain (45% for women and 36% for men) (seeTable 2).
Descriptive results and prevalence rates of multi-site are presented in Table 2. Older age employees comprised about 43% of the respondents. Over half the respondents reported high or moderate levels of job satisfaction. However, for those with low job satisfaction (41%), 67% reported multi-site pain. Although few (7%) employees reported poor work life balance, reporting of multi-site pain was high (83%). For those exposed to high levels of psychosocial hazards (33%), 75% of respondents reported having multi-site pain. A similar pattern was found for those exposed to high levels of physical hazards. Around 15% of employees reported poor general health and about 28% of the employees had poor work ability. Only 10% of respondents reported excellent work ability.
3.2Work-related factors associated with multi-site pain
Table 3 shows bivariate and multivariate relationships between work-related variables and multi-site pain. All measures were significantly associated with multi-site pain in the bivariate model.
The strongest bivariate association among work-related factors was medium to high levels of physical hazards (PRR = 7.40, 95% CI = 5.28–10.37). Medium to high levels of psychosocial hazards were also strongly related to multi-site pain in the bivariate model (PRR for high psychosocial hazard = 5.90, 95% CI = 4.24–8.21). Model II found that with age, gender, work-related variables, job satisfaction and work life balance, the association of both physical and psychosocial hazards was reduced but remained statistically significant. However, the impact of older age and being female on multi-site pain became stronger. In the final model (Model III) general health and work ability variables were added to Model II, the association of physical hazard with multi-site pain was stronger (PRR for high physical hazards = 7.58, 95% CI = 4.89–11.77). However, the relationship between psychosocial factors and multi-site pain was reduced (PRR for high psychosocial hazard = 1.59, 95% CI = 1.00–2.57). Older age (PRR = 2.55, 95% CI = 1.80–3.59) and female employees (PRR = 2.09, 95% CI = 1.49–2.93) remained significantly associated. Job satisfaction was no longer significantly associated with multi-site pain in the final model but poor work life balance remained a predictor variable (PRR = 2.33, 95% CI = 1.06–5.14).
Good or poor general health (PRR = 2.26/5.95, 95% = 1.60–3.19/3.43–10.31, respectively) and poor work ability (PRR = 2.73, 95% CI = 1.41–5.26) were also significantly related to a higher likelihood of reporting multi-site pain.
4Discussion
The aim of the current study was to determine prevalence and work-related determinants of multi-site musculoskeletal pain. A secondary aim was to explore potential age and gender differences in reporting of multi-site pain amongst employees in three Australian health care sector organisations. A high prevalence of musculoskeletal pain was found with 71% of respondents indicating pain in at least one body area. Point prevalence of multi-site pain in the study population was 52% (56% of women and 50% of men), (48% younger and 58% of older employees). Older employees and women were more likely to report multi-site pain. Those who were exposed to high levels of workplace physical and psychosocial hazards, poor work ability and work life balance were more likely to report multi-site pain.
Others have reported high prevalence of multi-site pain, although little has been described in the literature in relation to an Australian population [5, 10, 11, 15, 32]. The significant cultural and contextual issues around work-related pain mean the current study makes a useful contribution to the literature on multi-site pain. The relationship with older workers and increased prevalence of musculoskeletal pain has been reported previously but findings are inconsistent [14, 24]. The complex nature of musculoskeletal pain development is a likely contributing factor to these inconsistencies. Cumulative exposure to a range of hazards has been reported as a significant factor in predicting multi-site pain [10, 24]. In the current study employment history, a possible proxy for hazard exposure, was not recorded and as such cannot be explored more fully. However, the significant relationship between age and multi-site pain is of interest in the context of an ageing workforce and the need to focus on prevention activities across the whole working life.
4.1Health work ability and multi-site pain
The significant relationship between poor general health with pain in multiple body sites in our study was not surprising [15, 37]. Our results suggests a graded relationship between impaired overall health and multiple sites pain consistent with other findings [7, 15]. A significant relationship between work ability and multi-site pain in our study is also consistent with findings of earlier research where poor work ability was a strong predictor of multi-site pain [5, 14, 15].
4.2Work-related factors and multi-site pain
Physical hazards were strongly associated with multi-site pain by more than seven fold for those exposed to high physical hazards and is consistent with other findings [24, 38]. In our study, psychosocial hazards were also associated with pain in multiple body sites in both bivariate and multivariate analysis. However, in the final model of multivariate analysis the association of psychosocial hazards reached only boarder line significance. This is somewhat unexpected as the significant influence of psychosocial factors on multi-site pain has been previously described [10, 32]. More specifically, a moderate relationship was reported in a cross sectional study of Greek employees, between workplace support and multi-site pain [10]. In contrast, a study of Finnish employees over a 4-year period examining psychosocial factors and multi-site pain found only a weak relationship between the two measures [24]. Further investigation into the measure of multi-site pain is required, in relation to the aforementioned studies the influence of culture may explain contribute to the reported findings.
Health care work has been identified as high risk for developing MSDs [34, 39]. Australian data on work-related injuries (which include MSDs) indicate that the health and community services sector have one of the highest worker’s compensation claims rates [40]. Workers in the healthcare sector undertake a range of physically and cognitively demanding tasks that have been linked to the development of MSDs [41, 42]. A weak association was found between multi-site pain and psychosocial factors in the multivariate analysis; however, those reporting high levels of psychosocial hazards also had a high prevalence of multi-sitepain.
Workplace risk management strategies should focus on identification of all relevant hazards and risks. Multi-site pain remains relatively unexplored, and further research is required to understand the complex relationship between workplace risk factors and the development of multi-site pain. The rapidly ageing workforce will place increasing pressure on employees to remain employed for longer; so reducing the incidence of all pain, to ensure workers have capacity to stay is an important part of developing successful workplace retention strategies [17]. A paucity of intervention-based research identifying successful retention strategies for older workers creates some knowledge gaps that need to be addressed [43]. Reduction of MSDs should be seen as a high priority in this context.
Study findings should be considered in the context of several methodological limitations. The cross-sectional design of the study does not allow inference of causal associations to be drawn. A relatively low response rate and no information on non-respondents may contribute to bias in the findings of our study. Information on covariates such as smoking, body mass index and physical activity of the study participants was not collected due to the limitations on data collection, others have reported these factors as important determinants of multi-site pain [44]. In addition, the presence of musculoskeletal pain could enhance employee awareness of physical demands and increase the likelihood of reporting such activities [10]. Negative affectivity or tendency for somatization was not measured, and may influence participant reporting behavior. The perception of pain and other exposure variables were measured through self-administered questionnaires, no clinical measurement of pain were used. Recall bias was possible but the risk reduced due to the time frame of pain reporting (during the last sixmonths).
5Conclusion
This cross-sectional study found a higher prevalence of multi-site musculoskeletal pain compared to single-site pain among Australian health care sector employees. In addition, workplace physical and psychosocial hazards and poor work life balance were related to multi-site pain. Older employees and women were also more likely to report multi-site pain. In the context of an ageing population reduction of multi-site pain is important to maximize opportunities for workers to remain actively employed. Accurate identification of all relevant hazards and risks for multi-site pain is a critical first step in achieving this.
Conflict of interest
None declared.
Acknowledgments
This research is supported in part through a Development Grant from WorkSafe Victoria and the Transport Accident Commission (TAC), through the Institute for Safety, Compensation and Recovery Research (ISCRR).
References
[1] | Tsang A , von Korff M , Lee S , et al . Common chronic pain conditions in developed and developing countries: Gender and age differences and co-morbidity with depression-anxiety disorders. J Pain (2008) ;9: :883–91. |
[2] | Haldeman S , Carroll L , Cassidy JD . Findings from the bone and joint decade 2000 to 2010 task force on neck pain and its associated disorders. J Occup Environ Med (2010) ;52: (4):424–7. |
[3] | Murray CJL , Ezzati M , Flaxman AD , et al . Comprenshive systematic analysis of global epidemiology: Definitions, methods, simplification of DALYs, and comparative results from the global burden of disease study 2010. Lancet (2012) ;380: :2063–66. |
[4] | Carenes D , Parsons S , Ashby D , Breen A , Foster NE , Pincus T , Voget S , Underwood M . Chronic musculoskeletal pain rarely present in a single body sites: Results from a UK population study. Rheumatology (Oxford) (2007) ;46: (7):1168–70. |
[5] | Neupane S , Virtanen P , Leino-Arjas P , Miranda H , Siukola A , Nygård C-H . Multi-site pain and working conditions as predictors of work ability in a 4-year follow-up among food industry employees. Eur J Pain (2013) ;17: :444–51. |
[6] | Schmidt CO , Baumeister SE . Simple patterns behind complex spatial pain reporting? Assessing a classification of multi-site pain reporting in the general population. Pain (2007) ;133: :174e82. |
[7] | Kamaleri Y , Natvig B , Ihlebaek CM , Bruusqaard D . Localized or widespread musculoskeletal pain: Does it matter? Pain (2008) ;138: :41–6. |
[8] | Macdonald W , Oakman J . Musculoskeletal disorders: Using the evidence to guide practice. Journal of Health and Safety Research and Practice (2013) ;5: (2):7–12. |
[9] | Parot-Schinkel E , Descatha A , Ha C , Petit A , Leclerc A , Roquelaure Y . Prevalence of multisite musculoskeletal symptoms: A French cross-sectional working population-based study. BMC Musculoskeletal Disorders (2012) ;13: :122. |
[10] | Solidaki E , Chatzi L , Bitsios P , Markatzi I , Plana E , Castro F , Palmer K , Coggon D , Koqevinas M . Work-related and psychological determinants of multisite musculoskeletal pain. Scand J Work Environ Health (2010) ;36: :54–61. |
[11] | Yeung SS , Genaidy A , Deddens J , Alhemood A , Leung PC . Prevalence of musculoskeletal symptoms in single and multiple body regions and effects of perceived risk of injury among manual handling workers. Spine (2002) ;27: :2166–72. |
[12] | Natvig B , Eriksen W , Bruusgaard D . Low back pain as a predictor of long-term work disability. Scand J Public Health (2002) ;30: :288e92. |
[13] | Jordan KP , Kadam UT , Hayward R , Porcheret M , Young C , Croft P . Annual consultation prevalence of regional musculoskeletal problems in primary care: An observational study. BMC Musculoskelet Disord (2010) ;11: :144. |
[14] | Miranda H , Kaila-Kangas L , Heliövaara M , Leino-Arjas P , Haukka E , Liira J , Viikari-Juntura E . Musculoskeletal pain at multiple sites and its effects on work ability in a general working population. Occup Environ Med (2010) ;67: :449–55. |
[15] | Kamaleri Y , Natvig B , Ihlebaek CM , Bruusqaard D . Does the number of musculoskeletal pain sites predict work disability? A 14-year prospective study. Eur J Pain (2009) ;13: :426–30. |
[16] | Woolf AD , Pfleger B . Burden of major musculoskeletal conditions. Bull World Health Organ (2003) ;81: :646–56. |
[17] | Härmä M . Adding more years to the work careers of an aging workforce- What works? Scand J Work Env Health (2011) ;37: (6):451–3. |
[18] | Oakman J , Wells Y . Retirement Intentions: What is the role of push factors in predicting retirement intentions? Ageing & Society (2013) ;33: (6):998–1008. |
[19] | Coggon D , Ntani G , Palmer KT , et al . Patterns of multisite pain and associations with risk factors. Pain (2013) ;154: :1769–77. |
[20] | Hotopp U . The ageing workforce: A health issue. Economics and Labor Market Review (2007) ;1: (2):30–35. |
[21] | Taimela S , Läära E , Malmivaara A , Tiekso J , Sintonen H , Justen S , Aro T . Self-reported health problems and sickness absence in different age groups predominantly engaged in physical work. Occup Environ Med (2007) ;64: (11):739–46. |
[22] | Silverstein M . Meeting the challenges of an aging workforce. Am Jr Ind Med (2008) ;51: :269–80. |
[23] | Ilmarinen J . Physical requirements associated with the work of ageing workers in the European Union. Experimental Ageing Research (2002) ;28: :7–32. |
[24] | Neupane S , Miranda H , Virtanen P , Siukola A , Nygård C-H . Do physical or psychosocial factors at work predict multi-site musculoskeletal pain? A 4-year follow-up study in an industrial population. Int Arch Occup Environ Health (2013) ;86: :581–9. |
[25] | Alexopoulos EC , Stathi I-C , Charizani F . Prevalence of musculoskeletal disorders in dentists. BMC Musculoskeleta Disord (2004) ;5: :16. |
[26] | Solidaki E , Chatzi L , Bitsios P , Coggon D , Palmer KT , Kogevinas M . Risk factors for new onset and persistence of multi-site musculoskeletal pain in a longitudinal study of workers in Crete. Occup Environ Med (2013) ;69: :485–92. |
[27] | Cho NH , Kim I , Lim SH , Kim HA . Prevalence of widespread pain and its influence on quality of life: Population study in Korea. J Korean Med Sci (2012) ;27: :16–21. |
[28] | Bongers PM , Kremer AM , Ter Laak J . Are psychosocial factors, risk factors for symptoms and signs of the shoulder, elbow, or hand/wrist? A review of the epidemiological literature. Am Jr Ind Med (2002) ;41: :315–42. |
[29] | Nahit ES , Hunt IM , Lunt M , Dunn G , Silman AJ , Macfarlane GJ . Effects of psychosocial and individual psychological factors on the onset of musculoskeletal pain: Common and site-specific effects. Ann Rheum Dis (2003) ;62: (8):755–60 . |
[30] | Macfarlane GJ , Pallewatte N , Paudyal P , Blyth FM , Coggon D , Crombez G , Linton S , Leino-Arjas P , Silman AJ , Smeets RJ , van der Windt D . Evaluation of work-related psychosocial factors and regional musculoskeletal pain: Results from a EULAR Task Force. Ann Rheum Dis (2009) ;68: (6):885–91 . |
[31] | Gerr F , Fethke NB , Merlino L . A prospective study of musculoskeletal outcomes among manufacturing workers: I. effects of physical risk factors. Human Factors (2014) ;56: :112–30. |
[32] | Haukka E , Leino-Arjas P , Ojajärvi A , Takala EP , Viikari-Juntura E , Riihimäki H . Mental stress and psychosocial factors at work in relation to multi-site musculoskeletal pain: A longitudinal study of kitchen workers. Eur J Pain (2011) ;15: :432–38 . |
[33] | World Health Organization ((1993) ) Capacity, Report of a WHO Study Group. WHO Technical Series no 835. WHO: Geneva. |
[34] | Oakman J , Macdonald W , Wells Y . Developing a comprehensive approach to risk management of musculoskeletal disorders in non-nursing health care sector employees. Appl Ergon (2014) ;45: (6):1634–40. |
[35] | Griffiths A , Cox T , Karanika M , Khan S , Tomas J-M . Work design and management in the manufacturing sector: Development and validation of the Work Organisation Assessment Questionnaire. Occup Environ Med (2006) ;63: (10):669–75. |
[36] | Tabachnick BG and Fidell LS , (2005) Using Multivariate Statistics . Fifth Ed. Harper Collins. New York. |
[37] | Thomas E , Peat G , Harris L , Wilkie R , Croft PR . The prevalence of pain and pain interference in a general population of older adults: Cross-sectional findings from the North Staffordshire Osteoarthritis Project (NorStOP). Pain (2004) ;110: :361–8. |
[38] | Harkness EF , Macfarlane GJ , Nahit E , Silman AJ , McBeth J . Mechanical injury and psychosocial factors in the work place predict the onset of widespread body pain. Arthritis Rheum (2004) ;50: :1655–64. |
[39] | Tuller J , Brewer S , Amick BC III , Irvin E , Mahood Q , Pompeii LA , Wanq A , Van Eerd D , Gimeno D , Evanoff B . Occupational safety and health intervention to reduce musculoskeletal symptons in the health care sector. J Occup Rehab (2010) ;20: (1):199–219. |
[40] | Safe Work Australia (2012) . Compendium of Workers’ Compensation Statistics Australia 2010-11. Canberra, Australia: Retrieved July 2013 from: http://www.safeworkaustralia.gov.au/sites/swa/about/publications/pages/compendium-2010-11. |
[41] | Fray M , Hignett S . TROPHI: Development of a tool to measure complex, multi-factorial patient handling interventions. Ergonomics (2013) ;56: (8):1280–94. |
[42] | Long MH , Johnston V , Bogossian F . Work-related upper quadrant musculoskeletal disorders in midwives, nurses and physicians: A systematic review of risk factors and functional consequences. Appl Ergon (2012) ;43: (3):455–67. |
[43] | Cloostermans L , Bekkers MB , Uiters E , Proper KI . The effectiveness of interventions for ageing workers on (early) retirement, work ability and productivity: A systematic review. Int Arch Occup Environ Health (2014) ;88: (5):521–32. |
[44] | Haukka E , Ojajärvi A , Takala EP , Viikari-Juntura E , Leino-Arjas P . Physical workload, leisure-time physical activity, obesity and smoking as predictors of multisite musculoskeletal pain. A 2-year prospective study of kitchen workers. Occup Environ Med (2012) ;69: :485–92. |
Figures and Tables
Fig.1
Different anatomical area of body.
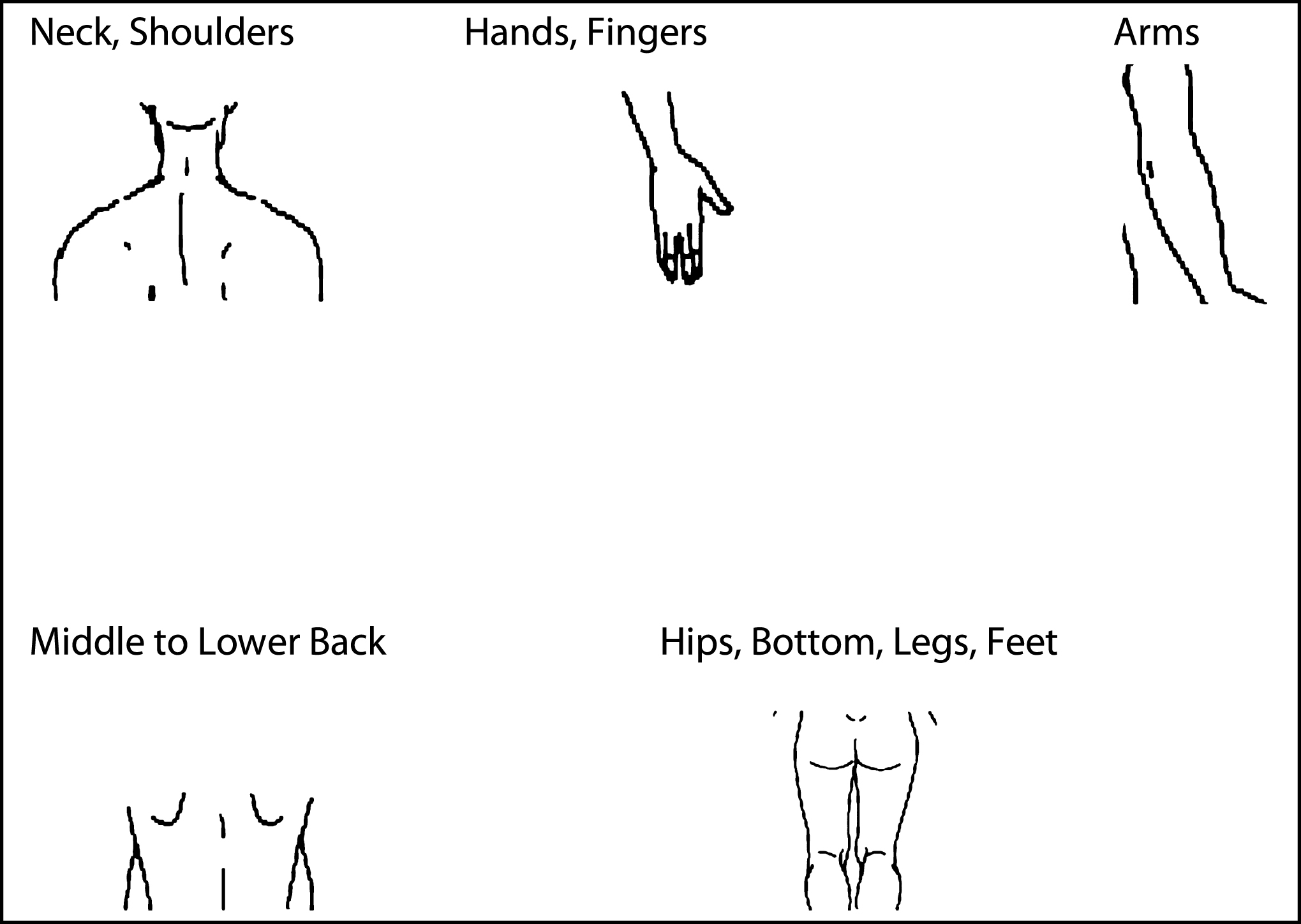
Table 1
Prevalence of localized and multiple site pain during the last six month by gender and age group
| All | Women | Men | p-value§ | Younger | Older | p-value§ | |||||
| N = 1348 (%) | N = 601 | % | N = 733 | % | N = 754 | % | N = 563 | % | |||
| Pain site | |||||||||||
| Neck, shoulder | 528 (39.1) | 262 | 44.3 | 264 | 36.2 | 0.002 | 302 | 40.4 | 217 | 38.9 | 0.307 |
| Hands, fingers | 648 (48.5) | 300 | 50.5 | 341 | 46.8 | 0.098 | 318 | 42.5 | 314 | 56.3 | <0.001 |
| Arms | 654 (49.1) | 287 | 48.7 | 361 | 49.5 | 0.409 | 328 | 43.9 | 311 | 56.1 | <0.001 |
| Middle/lower back | 553 (41.3) | 261 | 43.9 | 291 | 39.8 | 0.076 | 317 | 42.2 | 226 | 40.4 | 0.284 |
| Hips, bottom, legs | 540 (40.2) | 269 | 44.8 | 266 | 36.4 | 0.001 | 259 | 34.4 | 265 | 47.6 | <0.001 |
| Multi-site pain | 0.012 | 0.003 | |||||||||
| No pain | 314 (29.1) | 115 | 24.3 | 194 | 32.6 | 188 | 31.1 | 117 | 26.1 | ||
| One-site pain | 200 (18.6) | 94 | 19.9 | 106 | 17.8 | 129 | 21.3 | 70 | 15.6 | ||
| Multi-site pain | 564 (52.3) | 264 | 55.8 | 295 | 49.6 | 288 | 47.6 | 262 | 58.4 | ||
| Missing | 270 | 130 | – | 138 | – | 155 | – | 113 | – | ||
§ P-value obtained from chi-square test. Significant result are shown in bold.
Table 2
Distribution of study variables in total sample and by multi-site pain
| Characteristics | Total sample | Multi-site pain | P-value§ | ||
| N = 1348 | % | N = 564 | % | ||
| Age (Years) | <0.001 | ||||
| <45 | 753 | 57.3 | 288 | 47.6 | |
| ≥ 45 | 562 | 42.7 | 262 | 58.4 | |
| Gender | 0.025 | ||||
| Male | 732 | 55.0 | 295 | 49.6 | |
| Female | 600 | 45.0 | 264 | 55.8 | |
| Job satisfaction | <0.001 | ||||
| High | 163 | 12.1 | 33 | 25.4 | |
| Medium | 632 | 47.0 | 230 | 46.3 | |
| Low | 551 | 40.9 | 301 | 66.7 | |
| Work life balance | <0.001 | ||||
| High | 764 | 56.8 | 250 | 41.1 | |
| Medium | 484 | 36.0 | 245 | 63.5 | |
| Low | 98 | 7.3 | 68 | 82.9 | |
| Psychosocial hazard | <0.001 | ||||
| Low | 427 | 33.3 | 113 | 33.4 | |
| Medium | 432 | 33.6 | 165 | 48.7 | |
| High | 425 | 33.1 | 264 | 74.8 | |
| Physical hazard | <0.001 | ||||
| Low | 480 | 36.6 | 109 | 28.9 | |
| Medium | 444 | 33.9 | 200 | 56.7 | |
| High | 387 | 29.5 | 241 | 75.1 | |
| General health | <0.001 | ||||
| Very good | 643 | 48.0 | 178 | 35.0 | |
| Good | 498 | 37.2 | 235 | 60.7 | |
| Poor | 198 | 14.8 | 148 | 83.6 | |
| Work ability | <0.001 | ||||
| Excellent | 132 | 10.1 | 33 | 30.8 | |
| Good | 195 | 14.9 | 165 | 38.2 | |
| Moderate | 613 | 47.0 | 198 | 61.1 | |
| Poor | 365 | 28.0 | 148 | 79.6 | |
§ P-value obtained from chi-square test. Significant result are shown in bold.
Table 3
Prevalence rate ratios (PRR) with their 95% confidence intervals (CI) for multi-site pain due to various factors
| Characteristics | PRR, 95% CI | ||
| Model I | Model II | Model III | |
| Age (Years) | |||
| <45 | 1.0 | 1.0 | 1.0 |
| ≥ 45 | 1.54 (1.20–1.97) | 2.73 (1.98–3.77) | 2.55 (1.80–3.59) |
| Gender | |||
| Male | 1.0 | 1.0 | 1.0 |
| Female | 1.28 (1.00–1.67) | 1.98 (1.44–2.71) | 2.09 (1.49–2.93) |
| Job Satisfaction | |||
| High | 1.0 | 1.0 | 1.0 |
| Medium | 2.53 (1.64–3.90) | 1.45 (0.87–2.43) | 1.18 (0.67–2.07) |
| Low | 5.89 (3.79–9.16) | 2.21 (1.22–4.01) | 1.52 (0.79–2.92) |
| Work life balance | |||
| High | 1.0 | 1.0 | 1.0 |
| Medium | 2.49 (1.91–3.25) | 1.46 (1.03–2.06) | 0.96 (0.66–1.40) |
| Low | 6.97 (3.83–12.67) | 2.98 (1.45–6.12) | 2.33 (1.06–5.14) |
| Psychosocial hazard | |||
| Low | 1.0 | 1.0 | 1.0 |
| Medium | 1.88 (1.38–2.57) | 1.16 (0.79–1.70) | 1.12 (0.74–1.68) |
| High | 5.90 (4.24–8.21) | 2.13 (1.36–3.33) | 1.59 (1.00–2.57) |
| Physical Hazard | |||
| Low | 1.0 | 1.0 | 1.0 |
| Medium | 3.21 (2.36–4.36) | 3.10 (2.17–4.45) | 3.76 (2.53–5.57) |
| High | 7.40 (5.28–10.37) | 6.60 (4.41–9.88) | 7.58 (4.89–11.77) |
| General health | |||
| Very good | 1.0 | 1.0 | |
| Good | 2.87 (2.18–3.77) | 2.26 (1.60–3.19) | |
| Poor | 9.49 (6.12–14.70) | 5.95 (3.43–10.31) | |
| Work ability | |||
| Excellent | 1.0 | 1.0 | |
| Good | 0.89 (0.52–1.53) | 1.03 (0.52–2.05) | |
| Moderate | 2.20 (1.41–3.45) | 1.50 (0.83–2.71) | |
| Poor | 6.64 (4.08–10.78) | 2.73 (1.41–5.26) | |
Model I: Bivariate analysis. Model II: Work related factors adjusted for age and gender. Model III: Model II + general health and work ability. Significant result are shown in bold.




