Alternating Cystoscopy with Bladder EpiCheck® in the Surveillance of Low-Grade Intermediate-Risk NMIBC: A Cost Comparison Model
Abstract
BACKGROUND:
Bladder cancer surveillance is invasive, intensive and costly. Patients with low grade intermediate risk non-muscle invasive bladder cancer (NMIBC) are at high risk of recurrence.
OBJECTIVE:
The objective of this model is to compare the cost of a strategy to alternate surveillance with cystoscopy and a urine marker, Bladder EpiCheck, to standard surveillance.
METHODS:
A decision tree model was built using TreeAge Pro Healthcare to compare standard surveillance (Standard) with a modified surveillance incorporating Bladder EpiCheck. The model was based on 2 years of surveillance. Outcomes were obtained from literature. Costs were obtained from US and 9 European countries. Sensitivity analyses were performed.
RESULTS:
The efficacy of the model was equivalent in terms of recurrence for each arm with median recurrence rate of 22%. When setting marker price at 200 local currency, the marker arm was less expensive in the USA, Netherlands, Switzerland, Belgium, Italy, Austria and UK by 154€ to 329£ per patient, for a 2-year period. Cost was higher in France, Spain, and Germany by 33–103€. Cost parity was achieved with marker price between 148€ and $421. Marker cost and specificity have the greatest impact on the overall model cost.
CONCLUSIONS:
A strategy alternating the urine marker Bladder EpiCheck with cystoscopy in the surveillance of patients with low grade intermediate risk bladder cancer is cost equivalent in the US and European countries when the marker is priced 148€ –$421, as a result of the marker’s high specificity (86%). Prospective studies will be necessary to validate these findings.
INTRODUCTION
Bladder cancer is the 5th most common cancer and one of the most expensive from diagnosis to death. Approximately 75% of newly diagnosed bladder cancers are non-muscle invasive bladder cancer (NMIBC) and these are managed with risk-based intravesical therapy. Due to high risk of recurrence, patients with NMIBC undergo frequent cystoscopy to allow for earlier detection of recurrence and progression. Frequent cystoscopy is associated with cost and morbidity to patients [1–3]. There are also studies that demonstrate overuse of cystoscopy in low risk patients [4]. For patients with intermediate and high risk NMIBC, patients are often subjected to cystoscopy every 3 months for 1st one to two years [5]. The Bladder Cancer Advocacy Network Patient Survey Network evaluated research prioritization for patients and found that reducing pain associated with cystoscopy was high priority for patients with NMIBC [6]. As such, strategies to reduce number of cystoscopic procedures during surveillance would be viewed favorably if it can be done safely and efficiently.
Urine based tumor markers have been introduced to improve detection and surveillance of bladder cancer but their incorporation into clinical practice has been challenging. Overall, they have a better sensitivity than cytology especially for detection of low-grade cancers [7].
Bladder EpiCheck® (Nucleix Ltd.) is a new promising urine-based test which includes a panel of 15 DNA methylation patterns for the identification of recurrent NMIBC [8]. A recent study including 822 patients with NMIBC found the test had a specificity of 85.8% (95% confidence interval [CI] 83%–89%), a negative predictive value (NPV) of 94.3% (95% CI 92%–96%) for the detection of any cancer and an NPV of 98.8% (95% CI 97%–100%) for the detection of high-grade cancer [9, 10]. The sensitivity of the test was 62.5% (95% CI 51%–73%), 86.4% (95% CI 72.6%;94.8%) and 33.3% (95% CI 19%–51%) overall, high and low-grade cancer, respectively.
For patients with low grade intermediate risk NMIBC, the risk of recurrence is high but risk of progression is very low over a 3 to 6-month period [11]. For these patients, incorporating a urine marker alternating with cystoscopy could reduce the frequency of cystoscopy without jeopardizing oncologic outcomes. In this study, we develop a decision analysis model to compare standard surveillance with a modified surveillance incorporating Bladder EpiCheck. We assessed the cost of each approach in the US and several European countries.
MATERIALS AND METHODS
A decision tree model was built using TreeAge Pro Healthcare (Williamstown, MA) software to compare standard surveillance (Standard) with a modified surveillance incorporating Bladder EpiCheck where cystoscopy is alternated with Bladder EpiCheck test (marker). The model was based on 2 years of surveillance after a transurethral resection of a bladder tumor (TURBT). Table 1 details all model assumptions.
Table 1
Model assumptions
| Efficacy assumptions | |
| 1. Timing of cystoscopy | a. Patients in both arms (standard and marker) undergo cystoscopy at 3 months visit after a resection due to primary diagnosis or recurrence |
| b. If a patient in either arm has 2 consecutive negative surveillance visits in 3-months intervals (at 3 months and 6 months post resection), then switch to surveillance at 6-months intervals. | |
| c. Every recurrence resets the surveillance intervals to 3-months intervals | |
| d. Every patient underwent a 2-year cystoscopy since model was designed for a 2-year end point. | |
| 2. Efficacy of cystoscopy | All cystoscopic procedures were white light with 100% sensitivity and specificity. We recognize that sensitivity of cystoscopy is not 100% for low grade papillary tumors based on literature for enhanced cystoscopy, however, the literature regarding rate of recurrence and progression of intermediate risk NMIBC is all based on use of white light cystoscopy and there is insufficient data regarding long term follow up based on enhanced cystoscopy to develop a model. This assumption is equivalent for both arms in the study[26]. |
| 3. Cytology utilization | Use of cytology was included based on estimated utilization in each country (Table 2). |
| 4. Surveillance and treatment flow | In the marker arm, a surveillance visit with cystoscopy is followed by a 3-month surveillance visit with a Bladder EpiCheck test. If the test is negative then the patient’s next surveillance is with cystoscopy. If the test is positive then the patient undergoes an immediate cystoscopy. |
| A patient with a positive marker has 2 possible outcomes. If the patient has a recurrence then the marker was a true positive and they undergo a TURBT. Their next surveillance is 3 months later with cystoscopy. If the cystoscopy is negative then the patient had a false positive and it is considered a negative visit. | |
| Every recurrence is treated either by resection with TURBT or by fulguration. Use of fulguration was based on estimated rate of utilization in each country (Table 2). | |
| Formula: | |
| Marker positive: Sensitivity*(pRecurrence)+(1-Specificity)*((1- pRecurrence)) | |
| True positive = Sensitivity*pCancerRecur/((Sensitivity*pCancerRecur)+(1-Specificity)* (1-pCancerRecur)) | |
| False positive = 1 –probability of True Positive | |
| Patients with a negative marker do not undergo immediate cystoscopy. There are 2 possibilities. If the patient does not have cancer then they have a true negative. Their next follow up is a cystoscopy. If the patient has a missed cancer then they have a false negative marker. At next surveillance cystoscopy, they will have cancer rate equivalent to the probability of a missed cancer in addition to risk of new cancer developing (probability of cancer) at that timepoint. | |
| Formula: | |
| Marker Negative: Specificity*(1-pRecurrence)+(1-Sensitivity)*(pRecurrence) | |
| True Negative: Specificity*(1-pRecurrence)/((Specificity*(1-pRecurrence))+(1-Sensitivity)*pRecurrence) | |
| False Negative = 1 –probability of True Negative | |
| 5. Recurrence rate | The cancer recurrence rate varies at different time points of surveillance with highest rate at 3 months after TURBT [11]. The rate of recurrence at 3 months after TURBT was set at 10%. The absolute rates at 6, 9 and 12 months were 3.3% and 15, 18, 21 and 24 months were 2.5%. This resulted in overall rate of up to 30% over 2 years |
| 6. Progression rate | In the model we assume that all recurrences are low grade. The rate of progression to high grade disease is around 1-2% per year so the impact on cost would be very low. The rate would be equivalent in both arms so unlikely to bias model. |
| 7. Marker performance | Sensitivity and specificity for Bladder EpiCheck based on most recent results of a multicenter trial of 822 patients was 33.3% sensitivity for low grade and 85.8% specificity |
| Cost assumptions | |
| 1. Procedures costs and fees | Costs for cystoscopy, cytology, pathology, professional fees and TURBT were obtained from health agencies and experts at US and various European countries (Table 2). |
| 2. Rate of procedures | The rate of cytology and fulguration varied per country and their rate of utilization in the model are depicted Table 2 |
| 3. Marker cost | Cost of the markers was 200 in each local currency |
| 4. Patient costs | Costs to patients included loss of work and travel. We assume that patients use 1\2 day of work for their visit if they undergo cystoscopy or fulguration and 2 days if they undergo TURBT. Travel costs vary per country but we assumed a cost of 10$ in US or 10€ to include transportation and parking. |
| Average wage in 2018 for all countries were obtained from the OECD statistics website https://stats.oecd.org/Index.aspx?DataSetCode=AV_AN_WAGE The annual average wage was obtained by dividing the national-accounts-based total wage bill by average number of employees in the total economy, which was then multiplied by the ratio of the average usual weekly hours per full-time employee to the average usual weekly hours for all employees. To extrapolate average daily wage, we assumed there are 20 work days per month and 8 work hours per day. |
Table 2
Model costs and rates of use of cytology and office fulguration
| Country | Austria | Belgium | France | Germany | Italy | The Netherlands | Spain | Switzerland | UK | USA |
| % cytology | 100% | 50% | <15% | 100% | 50–100% (75%)* | 0 | 30% | 15% | 30% | 100% |
| % fulguration | 0 | <20% (20%)* | 0 | 0 | <10% (10%)* | 0 | 20% | 0 | 0 | 20% |
| Procedure cost | ||||||||||
| Source | hospital costs | social security | Social security | Reimburse-ment | hospital costs | Reimburse-ment | hospital costs | Tarmed, pathology | NHS tariffs | CPT codes |
| Currency | Euro€ | Euro€ | Euro€ | Euro€ | Euro€ | Euro€ | Euro€ | CHF | Pound£ | USD$ |
| Cystoscopy | 183.72 | 205.9 | 99 | 94.85 | 230 | 291.33 | 96 | 250 | 330 | 242.92∧ |
| Cytology | 49.14 | 20 | 96 | 14.72 | 60 | 0‡ | 20 | 100 | 17 | 100 |
| Fulguration | 334.19 | 75 | NA | NA | 1,148 | NA | 600 | NA | 935 | 703.5 |
| TURBT | 1,914 | 750 | 3,000 | 2,600 | 1,628.8 | 5,017.11 | 1,600 | 7,000 | 3,533.5 | 3,047.5 |
| Pathology | 210.77 | 68.7 | 35 | 65 | 230 | 0‡ | 219 | 250 | 0 | 269.88 |
| Patient costs | ||||||||||
| Transportation | 10 | 10 | 10 | 10 | 10 | 10 | 10 | 10 | 10 | 10 |
| Annual average income | 43,468 | 45,097 | 38,280 | 40,522 | 29,601 | 47,422 | 27,946 | 87,716 | 35,978 | 63,093 |
| Average hourly income | 22.64 | 23.49 | 19.94 | 21.11 | 15.42 | 24.70 | 14.56 | 45.69 | 18.74 | 32.86 |
*Rate used in model. ∧Based on mixed payers from over 1,200 cystoscopic procedures at UT Southwestern Medical Center in Dallas. ‡Cytology and pathology costs are included in the overall price of the procedure (cystoscopy and TURBT, respectively).
The base case is a patient with intermediate risk NMIBC according to the AUA guidelines for NMIBC with low grade only disease who is undergoing surveillance [5]. Intermediate risk patients with high grade Ta tumors were not included.
The initial year of the model is shown in supplementary Figures 1 and 2.
Sensitivity analysis
In one-way sensitivity analysis, costs and medical assumptions were individually adjusted across a range of values to assess the impact of one variable on baseline assumptions. A tornado diagram was developed to evaluate the relative impact of different cost components (Fig. 1). Two-way sensitivity analyses were performed evaluating the least costly approach when vary 2 factors over a range (Figs. 2 and 3).
Fig. 1
Tornado diagram using U.S. model evaluating incremental cost of Standard and Marker arms.
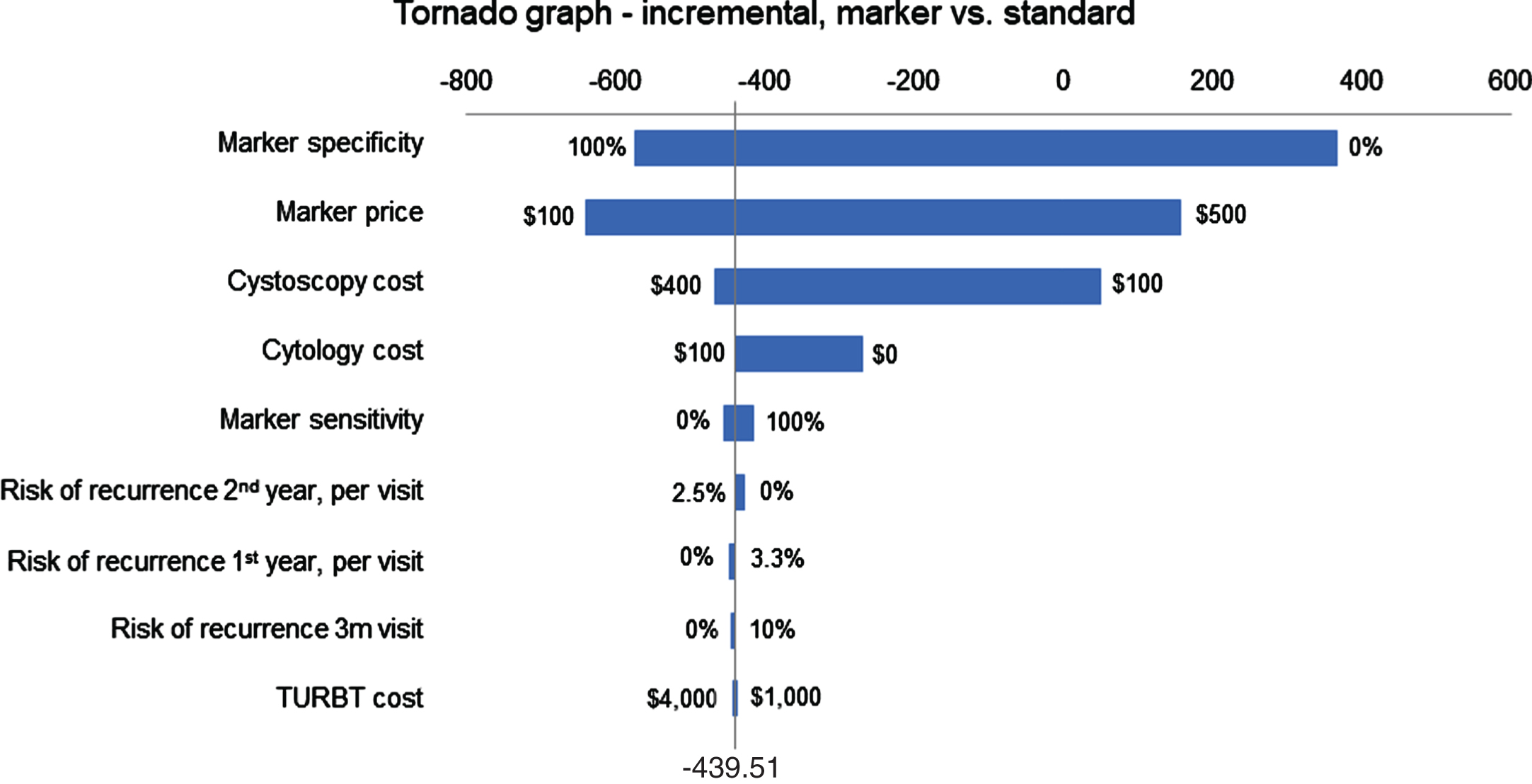
Fig. 2
Two-way sensitivity analysis based on US model evaluating cost parity with varying cost of marker ($) and specificity of marker. The red area represents the area where the standard is less costly and the blue area is the area where the marker is less costly. The margin between these areas represent points where the costs are the same in both arms.
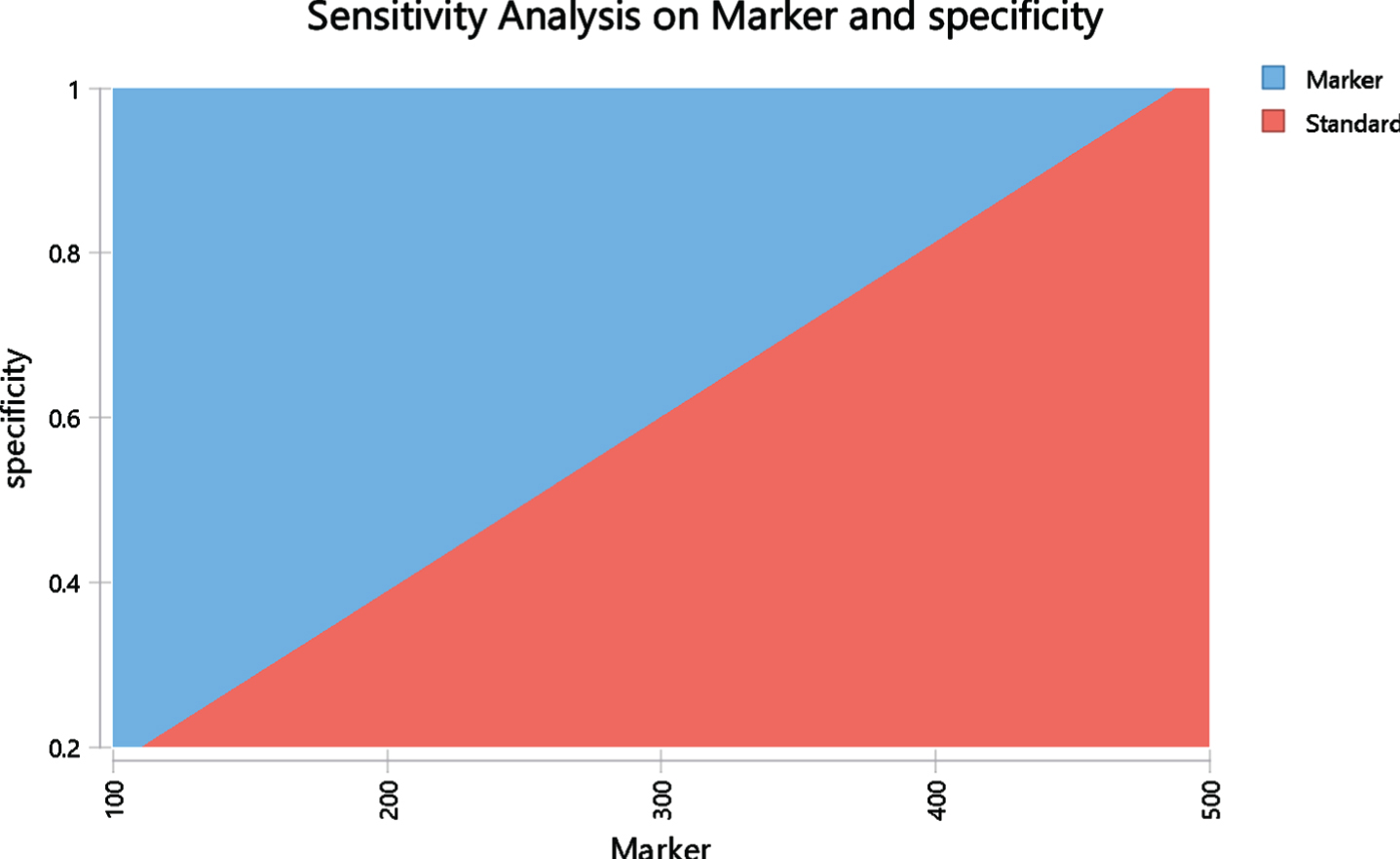
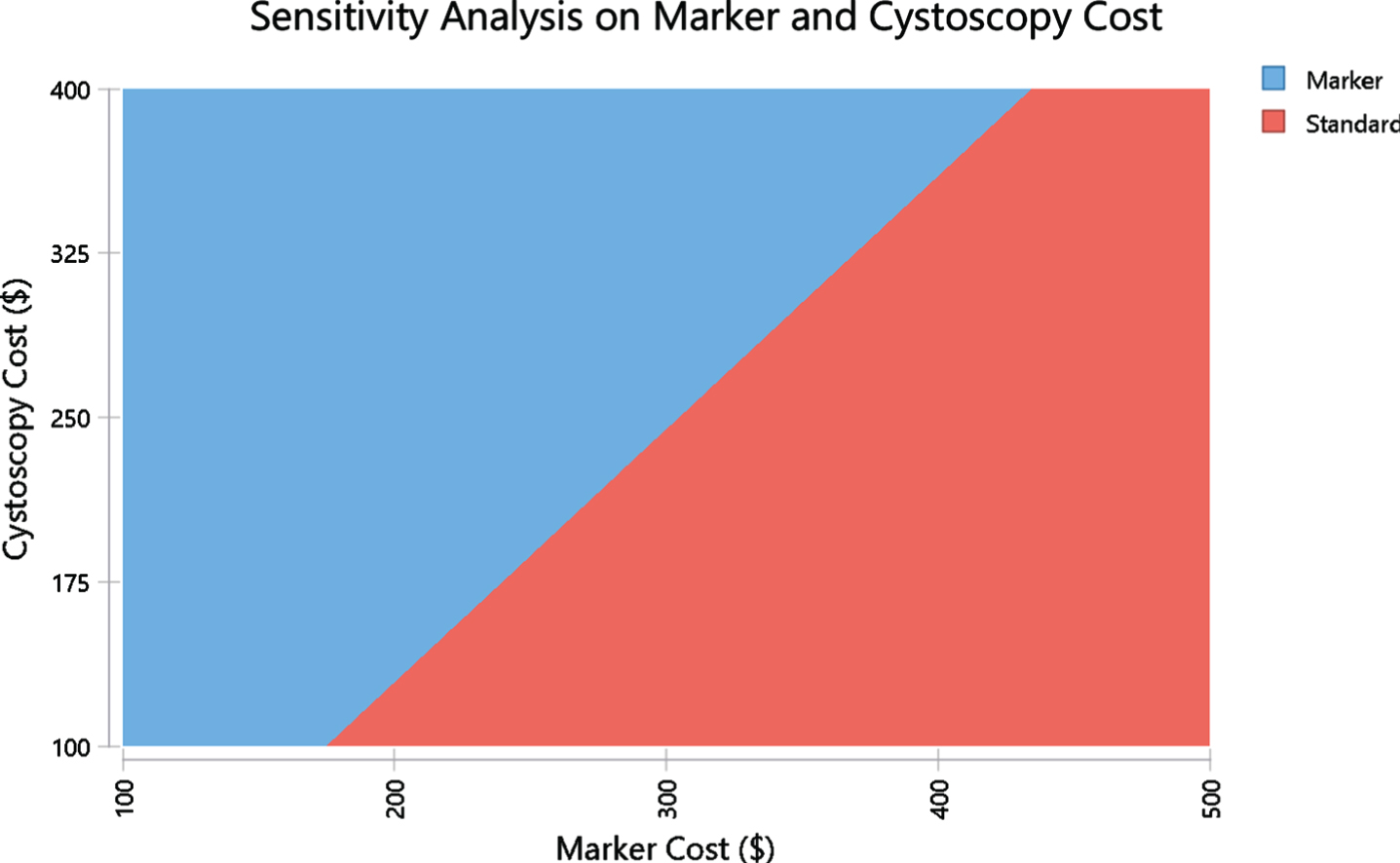
Fig. 3
Two-way sensitivity analysis based on US model evaluating cost parity with varying cost of marker ($) and cost of cystoscopy ($). The red area represents the area where the standard is less costly and the blue area is the area where the marker is less costly. The margin between these areas represent points where the costs are the same in both arms.
RESULTS
The efficacy of the model was equivalent in terms of recurrence for each arm with median recurrence rate of 22%. The cost of each arm varied by country (Table 3). When assuming marker cost of 200 local currency, the marker arm was less expensive in the USA, Netherlands, Switzerland, Belgium, Italy, Austria and UK by 154€ to 329£ per patient for the 2-year period. Cost was slightly higher in France, Spain, and Germany by 33–103€ under the same assumptions. The marker cost parity point represents the cost of the marker at which the marker and standard arms are cost equivalent for each country (Table 3), and was between 148€ in Spain and $421 in the USA. The tornado diagram (Fig. 1) shows the impact of different factors on cost of different arms of the model (based on USA costs). Marker cost and specificity have the greatest impact on the overall model cost. A higher marker price leads to increase in marker arm costs. A lower specificity also increases cost since more patients in the marker arm require cystoscopy due to false positive results. The cost of cystoscopy is also an important factor since it impacts the standard arm cost more than marker arm.
Table 3
Outcomes of model and marker cost parity point
| Country | Austria | Belgium | France | Germany | Italy | Netherlands | Spain | Switzerland | UK | USA |
| Currency | Euro€ | Euro€ | Euro€ | Euro€ | Euro€ | Euro€ | Euro€ | CHF | Pound£ | USD$ |
| Marker arm | 2,100 | 1,730 | 1,775 | 1,789 | 2,051 | 2,977 | 1,390 | 3,743 | 2,699 | 2,805 |
| Standard arm | 2,277 | 1,884 | 1,697 | 1,757 | 2,252 | 3,273 | 1,287 | 4,141 | 3,028 | 3,244 |
| Difference | 177 | 154 | 78* | 33* | 201 | 296 | 103* | 399 | 329 | 439 |
| Marker cost parity point | 289 | 277 | 161 | 184 | 301 | 349 | 148 | 401 | 365 | 421 |
*Standard arm is less expensive than marker arm.
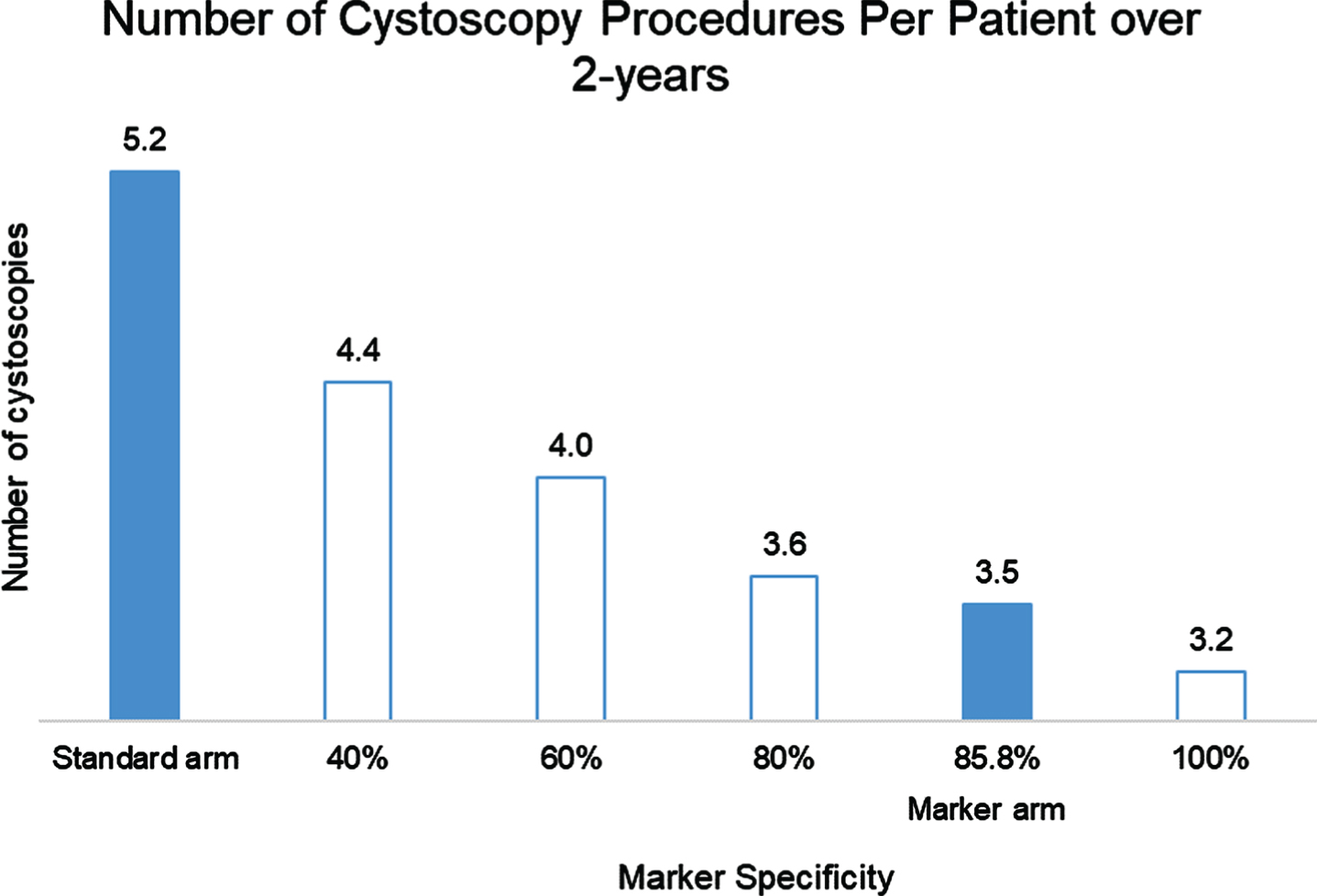
We evaluated the number of cystoscopy procedures in each arm varying the specificity in the marker arm. In the baseline model, the average number of cystoscopy procedures per patient performed over 2 years was 5.2 (Fig. 4). With a specificity of 85.8% for the marker, the average number of cystoscopy procedures was 3.5. Lower marker specificity is associated with a greater number of cystoscopy procedures in marker arm.
Fig. 4
Number of cystoscopy procedures per patient over 2 years in Standard and Marker arms.
One way sensitivity analysis found that in the U.S. model, the marker arm becomes more expensive than the standard arm in case the specificity is below 38.9% or if cystoscopy costs less than $129.4. On the other hand, marker sensitivity had minimal impact on its cost-effectiveness with merely $10 difference in the cost-parity price between sensitivity of 20% and 80%. Two-way sensitivity analyses were performed to assess if marker or standard is more costly when varying marker specificity and price (Fig. 2). The red area represents the area where the standard is less costly and the blue area is the area where the marker is less costly. The margin between these areas represent points where the costs are the same in both arms. For example, when the specificity is 80%, marker is less expensive as long as marker is priced below $395. If specificity drops by 20% to 60% then the maximum marker price for cost-saving drops by ∼25% below $300. A two-way sensitivity analysis was also performed evaluating marker and cystoscopy cost using US model. It demonstrates cost points for cystoscopy and the marker where each arm is less costly. At current marker cost of $200 and cystoscopy average cost of $242, the marker arm is less costly.
DISCUSSION
Low grade non-invasive bladder cancers are common and many of these tumors are categorized as intermediate risk due to frequent recurrences, increased size or multiplicity. These low grade tumors rarely progress to invasive or high grade disease. Most guidelines recommend frequent cystoscopy procedures to identify recurrent tumors but there is both a financial cost and patient discomfort associated with these procedures [12]. The use of urine-based tumor markers to reduce the number of procedures is a meritable goal. In this model, we evaluated the use of Bladder EpiCheck® (Nucleix Ltd.) to alternate with cystoscopy in the surveillance of low-grade non-invasive bladder cancers over a 2-year period of time. We evaluated the cost of a marker-based approach compared to a standard approach in 10 countries. When assuming marker cost of 200 local currency, the marker arm was less expensive in the USA, Netherlands, Switzerland, Belgium, Italy, Austria and UK. Cost was slightly higher in France, Spain, and Germany where reported cystoscopy costs were less than 100€. In these countries cost parity was achieved when marker was priced 148€–184€. The use of Bladder EpiCheck reduced frequency and number of cystoscopies as well as reducing costs over a 2-year period of time. For example, in the US, the average cost benefit per patient was $439 and the number of cystoscopies was 3.47 in the marker arm vs. 5.19 in the standard arm.
When considering an alternative strategy to cystoscopy, the most important consideration is safety. There are several reasons why using a low-grade intermediate risk cohort makes sense. First, progression of disease within 3 to 6 months is exceedingly rare for these patients. Intermediate risk low grade patients have EORTC progression scores of 2–6. These patients are estimated to have a 1% risk of progression at 1 year [11]. In our model, patients even in the marker arm had a cystoscopy every 6 months so missed progression would be very low. It is even rarer for a low-grade Ta tumor to progress to muscle invasive disease so at worst likely could become HG Ta. Furthermore, the sensitivity of Bladder EpiCheck for high grade disease is 86.4% (95% CI 72.6%;94.8%) and an NPV of 98.8% (95% CI 97%–100%) for the detection of high-grade cancer [9]. As such, over a one-year period less than 1 patient per 1,000 patients would have a 3 month delay in diagnosing a high grade cancer. Missing a low-grade cancer has minimal impact on patient outcomes and there are even studies suggesting conservative management of non-invasive low grade tumors [13–15]. Using a marker alternating with cystoscopy has the advantage of reducing patient discomfort while still detecting cancers within reasonable timeframes. In most countries, the marker-based approach was less expensive since the marker was less expensive than cystoscopy especially when one considers the accompanying loss of work. Only in 3 countries where the cost of cystoscopy was reported to be less than 100€ was the standard arm less expensive and marker price had to be reduced to 148–184€ to achieve cost parity.
Sensitivity analyses were performed to determine the cost at which both arms were cost-equivalent. In Table 3, the cost of the marker at which the 2 arms (standard and marker based) were cost-equivalent ranged from 148€ to $421. Two-way sensitivity analyses were performed using the US model to identify the impact of varying marker cost with marker specificity and cystoscopy cost. These can be performed for each country to determine the impact of varying costs and marker performance. The tornado diagram identified the factors that have the highest impact on cost of each arm. While sensitivity had a minimal impact overall, specificity significantly impacts the model since any patient with a positive marker undergoes cystoscopy. Those patients have the cost of the marker and the cost of cystoscopy. As such, a test that results in many false positive results can dramatically increase the cost of a marker arm. Since the Bladder EpiCheck test has a specificity of 85.8%, this is an infrequent event.
There have been several prior models published evaluating the use of markers in surveillance of bladder cancer [16, 17]. These models did not focus on low grade intermediate-risk disease but found that markers could be cost-effective if marker cost was reasonable and that several markers had sufficiently good performance characteristics. There is still need to perform prospective studies to evaluate the safety of such an approach as well as assessing patient and physician acceptance [18]. There is an ongoing study (UroFollow) in which patients with pTa G1/G2 NMIBC, a tumor size less than 3 cm, and with no accompanying pTis are randomized (1:1) to either usual-care with cystoscopy or the marker arm which includes a urine marker and ultrasound [19]. The primary endpoint of UroFollow is to investigate, if marker-guided (noninvasive) follow-up of patients with low- and intermediate-risk NMIBC is equally effective to detect tumor recurrence and progression compared to standard surveillance using cystoscopy.
There are some additional considerations when using a marker in surveillance. While we assumed that white light cystoscopy has a 100% sensitivity and specificity, this is not accurate since there are both false negative results as demonstrated from literature regarding enhanced cystoscopy as well as the risk for false positive findings [20–22] It is also possible that a positive marker result may improve urothelial carcinoma detection rate using cystoscopy as seen in the CeFub trial [23]. There is a risk of finding abnormal lesions by cystoscopy that are not cancerous which could result in unnecessary biopsies adding cost and morbidity to the patient [19, 24]. This was not incorporated into the model but would be reduced in patients in the marker arm.
In this analysis we did not include the indirect costs of cystoscopy’s complications, such as urinary tract infection, urinary retention, etc. which can result in antibiotic treatment in the community and additional loss of work in the mild cases, or prolong hospitalization in the severe ones [25]. This biases the cost result against the marker arm. There are also indirect benefits of avoiding use of office assistants and appointment slots for the urologist while a potential downside of reducing profits from the procedure. We did not assess a strategy of avoiding cystoscopy altogether with longer intervals between surveillance visits. While this would reduce patient visits, there is little data on risks and benefits and impact on quality of life. While a marker adds costs, there is a high sensitivity for high grade disease and it provides some reassurance that a longer interval between cystoscopy is safe.
There are some inherent limitations in developing models. The assumptions used were based on best available literature and cost data acquired from varying countries. The accuracy of cost data is sometimes difficult to ascertain especially in very heterogeneous health care systems. Sensitivity analyses help with analyzing the variance but future studies using real world data will be necessary to determine the actual cost if these types of strategies are implemented. Quality of life is also an important factor in patients with NMIBC. There are benefits to patients with avoiding cystoscopy since it is an invasive procedure but there are potential issues with anxiety among patients who get a marker due to lower sensitivity. However, the impact of these considerations on quality of life are unknown. Future studies should include specific and validated questionnaires to evaluate the impact of a marker based strategy on quality of life. There is also another potential benefit of a urine marker based approach due to the COVID 19 pandemic since use of urine tests may reduce visits to the health care system leading to lower risk of exposure of patients and medical staff. Another limitation of the model is that we did not include the cost of intravesical therapies. Many patients are given intravesical therapies for intermediate risk bladder cancers but rates vary by provider and geography. The cost of intravesical therapies would be equivalent for both arms of the model and would not impact the conclusions.
A strategy alternating the urine marker Bladder EpiCheck with cystoscopy in the surveillance of patients with low grade intermediate risk bladder cancer is cost-equivalent in the US and European countries when the marker is priced 148€–$421. Prospective studies will be necessary to validate these findings.
ACKNOWLEDGMENTS
The authors have no acknowledgments
FUNDING
This analysis was funded by Nucleix Ltd.
AUTHOR CONTRIBUTIONS
| Author | conception | performance of work | interpretation of data | writing the article | Access to the data |
| Yair Lotan | Yes | Yes | Yes | Yes | Yes |
| Georgios Gakis | No | Yes | Yes | Yes | No |
| Matteo Manfredi | No | Yes | Yes | Yes | No |
| Juan Morote | No | Yes | Yes | Yes | No |
| Hugh Mostafid | No | Yes | Yes | Yes | No |
| Francesco Porpiglia | No | Yes | Yes | Yes | No |
| Cedric Poyet | No | Yes | Yes | Yes | No |
| Morgan Roupret | No | Yes | Yes | Yes | No |
| Claude Schulman | No | Yes | Yes | Yes | No |
| Shahrokh Shariat | No | Yes | Yes | Yes | No |
| Johannes Alfred Witjes | No | Yes | Yes | Yes | No |
ETHICAL CONSIDERATIONS
This study, as a literature review is exempt from any requirement for Institutional Review Board approval.
CONFLICT OF INTERESTS
All authors are consultants for Nucleix Ltd (YL, GG, MM, JM, HM, FP, CP, MR, CS, SS, AW)
SUPPLEMENTARY MATERIAL
[1] Two figures are included in the supplementary material.
REFERENCES
[1] | Svatek RS , Hollenbeck BK , Holmäng S , Lee R , Kim SP , Stenzl A , Lotan Y . The economics of bladder cancer: costs and considerations of caring for this disease. Eur Urol. (2014) ;66: (2):253–62. |
[2] | Patel AR , Jones JS , Babineau D . Lidocaine 2% gel versus plain lubricating gel for pain reduction during flexible cystoscopy: a meta-analysis of prospective, randomized, controlled trials. J Urol. (2008) ;179: (3):986–90. |
[3] | Aaronson DS , Walsh TJ , Smith JF , Davies BJ , Hsieh MH , Konety BR . Meta-analysis: does lidocaine gel before flexible cystoscopy provide pain relief? BJU Int. (2009) ;104: (4):506–9; discussion 509-10. |
[4] | Han DS , Lynch KE , Chang JW , Sirovich B , Robertson DJ , Swanton AR , Seigne JD , Goodney PP , Schroeck FR . Overuse of Cystoscopic Surveillance Among Patients With Low-risk Non-Muscle-invasive Bladder Cancer - A National Study of Patient, Provider, and Facility Factors. Urology. (2019) ;131: :112–9. |
[5] | Chang SS , Boorjian SA , Chou R , Clark PE , Daneshmand S , Konety BR , Pruthi R , Quale DZ , Ritch CR , Seigne JD , Skinner EC , Smith ND , McKiernan JM . Diagnosis and Treatment of Non-Muscle Invasive Bladder Cancer: AUA/SUO Guideline. J Urol. (2016) ;196: (4):1021–9. |
[6] | Smith AB , Chisolm S , Deal A , Spangler A , Quale DZ , Bangs R , Jones JM , Gore JL . Patient-centered prioritization of bladder cancer research. Cancer. (2018) ;124: (15):3136–44. |
[7] | Soria F , D’Andrea D , Pohar K , Shariat SF , Lotan Y . Diagnostic, prognostic and surveillance urinary markers in nonmuscle invasive bladder cancer: any role in clinical practice? Curr Opin Urol. (2018) ;28: (6):577–83. |
[8] | Mancini M , Righetto M , Zumerle S , Montopoli M , Zattoni F . The Bladder EpiCheck Test as a Non-Invasive Tool Based on the Identification of DNA Methylation in Bladder Cancer Cells in the Urine: A Review of Published Evidence. Int J Mol Sci. (2020) ;21: (18):6542. |
[9] | Lozano F , Morote J , Leibovitch I , Cornel EB , Baard J , Gakis G , Alvarez-Maestro M , Van Valenberg H , Sternberg I , Willemsen E , Albers LF , Hegemann ML , Paitan Y , Witjes JA . Performance of Bladder EpiCheckTM forNMIBCmonitoring updated results of a European multi-center study. Poster #709 EAU2019 |
[10] | Witjes JA , Morote J , Cornel EB , Gakis G , van Valenberg FJP , Lozano F , Sternberg IA , Willemsen E , Hegemann ML , Paitan Y , Leibovitch I . Performance of the Bladder EpiCheck™ Methylation Test for Patients Under Surveillance for Non-muscle-invasive Bladder Cancer: Results of a Multicenter, Prospective, Blinded Clinical Trial. Eur Urol Oncol. (2018) ;1: (4):307–13. |
[11] | Sylvester RJ , van der Meijden AP , Oosterlinck W , Witjes JA , Bouffioux C , Denis L , Newling DW , Kurth K . Predicting recurrence and progression in individual patients with stage Ta T1 bladder cancer using EORTC risk tables: a combined analysis of 2596 patients from seven EORTC trials. Eur Urol. (2006) ;49: (3):466–5; discussion 475-7. |
[12] | Raskolnikov D , Brown B , Holt SK , Ball AL , Lotan Y , Strope S , Schroeck F , Ullman R , Lipman R , Smith AB , Gore JL . Reduction of Pain during Flexible Cystoscopy: A Systematic Review and Meta-Analysis. J Urol. (2019) ;202: (6):1136–42. |
[13] | Pruthi RS , Baldwin N , Bhalani V , Wallen EM . Conservative management of low risk superficial bladder tumors. J Urol. (2008) ;179: (1):87–90; discussion 90. |
[14] | Smith ZL , Soloway MS . Expectant Management of Low-Risk Bladder Cancer. Curr Urol Rep. (2015) ;16: (12):82. |
[15] | Hurle R , Lazzeri M , Vanni E , Lughezzani G , Buffi N , Casale P , Saita A , Morenghi E , Forni G , Cardone P , Lista G , Colombo P , Peschechera R , Pasini L , Zandegiacomo S , Benetti A , Maffei D , Vavassori I , Guazzoni G . Active Surveillance for Low Risk Nonmuscle Invasive Bladder Cancer: A Confirmatory and Resource Consumption Study from the BIAS Project. J Urol. (2018) ;199: (2):401–6. |
[16] | Lotan Y , Roehrborn CG . Cost-effectiveness of a modified care protocol substituting bladder tumor markers for cystoscopy for the followup of patients with transitional cell carcinoma of the bladder: a decision analytical approach. J Urol. (2002) ;167: (1):75–9. |
[17] | Nam RK , Redelmeier DA , Spiess PE , Sampson HA , Fradet Y , Jewett MA . Comparison of molecular and conventional strategies for followup of superficial bladder cancer using decision analysis. J Urol. (2000) ;163: (3):752–7. |
[18] | Lotan Y , Black PC , Caba L , Chang SS , Cookson MS , Daneshmand S , Kamat AM , McKiernan JM , Pruthi RS , Ritch CR , Steinberg GD , Svatek RS , Zwarthoff EC . Optimal Trial Design for Studying Urinary Markers in Bladder Cancer: A Collaborative Review. Eur Urol Oncol. (2018) ;1: (3):223–30. |
[19] | Benderska-Söder N , Hovanec J , Pesch B , Goebell PJ , Roghmann F , Noldus J , Rabinovic J , Wichert K , Gleichenhagen J , Käfferlein HU , Köhler CU , Johnen G , Kernig K , Hakenberg O , Jahn D , Todenhöfer T , Stenzl A , Gleissner J , Gerwert K , El-Mashtoly S , Behrens T , Brüning T , Schmitz-Dräger BJ . Towards non-invasive follow-up of low risk bladder cancer - Rationale and concept of the UroFollow trial. Urol Oncol. (2020) ;12: :886–95. |
[20] | Lotan Y , Bivalacqua TJ , Downs T , Huang W , Jones J , Kamat AM , Konety B , Malmström PU , McKiernan J , O’Donnell M , Patel S , Pohar K , Resnick M , Sankin A , Smith A , Steinberg G , Trabulsi E , Woods M , Daneshmand S . Blue light flexible cystoscopy with hexaminolevulinate in non-muscle-invasive bladder cancer: review of the clinical evidence and consensus statement on optimal use in the USA - update 2018. Nat Rev Urol. (2019) ;16: (6):377–86. |
[21] | Li K , Lin T , Fan X , Duan Y , Huang J . Diagnosis of narrow-band imaging in non-muscle-invasive bladder cancer: a systematic review and meta-analysis. Int J Urol.. (2013) ;20: (6):602–9. |
[22] | Svatek RS , Lee D , Lotan Y . Correlation of office-based cystoscopy and cytology with histologic diagnosis: how good is the reference standard? Urology. (2005) ;66: (1):65–8. |
[23] | van der Aa MNM , Steyerberg EW , Bangma C , van Rhijn BWG , Zwarthoff EC , van der Kwast TH . Cystoscopy revisited as the gold standard for detecting bladder cancer recurrence: diagnostic review Bias in the randomized,prospective CEFUB trial. J Urol. (2010) ;183: (1):76–80. |
[24] | Schmitz-Dräger C , Bonberg N , Pesch B , Todenhöfer T , Sahin S , Behrens T . Brüning T, Schmitz-Dräger BJ. Replacing cystosopy by urine markers in the follow-up of patients with low risk non muscle-invasive bladder cancer? - An IBCN project. Urol Oncol. (2016) ;34: :452–9. |
[25] | Turan H , Balci U , Erdinc FS , Tulek N , Germiyanoglu C . Bacteriuria, pyuria and bacteremia frequency following outpatient cystoscopy. Int J Urol. (2006) ;13: (1):25–8. |
[26] | Burger M , Grossman HB , Droller M , Schmidbauer J , Hermann G , Drăgoescu O , Ray E , Fradet Y , Karl A , Burgués JP , Witjes JA , Stenzl A , Jichlinski P , Jocham D . Photodynamic diagnosis of non-muscle-invasive bladder cancer with hexaminolevulinate cystoscopy: a meta-analysis of detection and recurrence based on raw data. Eur Urol.. (2013) ;64: (5):846–54. |




